Neuroendocrine neoplasms (NENs) are a heterogeneous group of tumours that most commonly arise in the digestive system or lungs, although they can develop in other parts of the body. These cancers begin in neuroendocrine cells, which are specialised cells found throughout the body.
Neuroendocrine cells play an important role in normal body function by producing, storing, and releasing hormones and small protein molecules that help regulate many physiological processes.
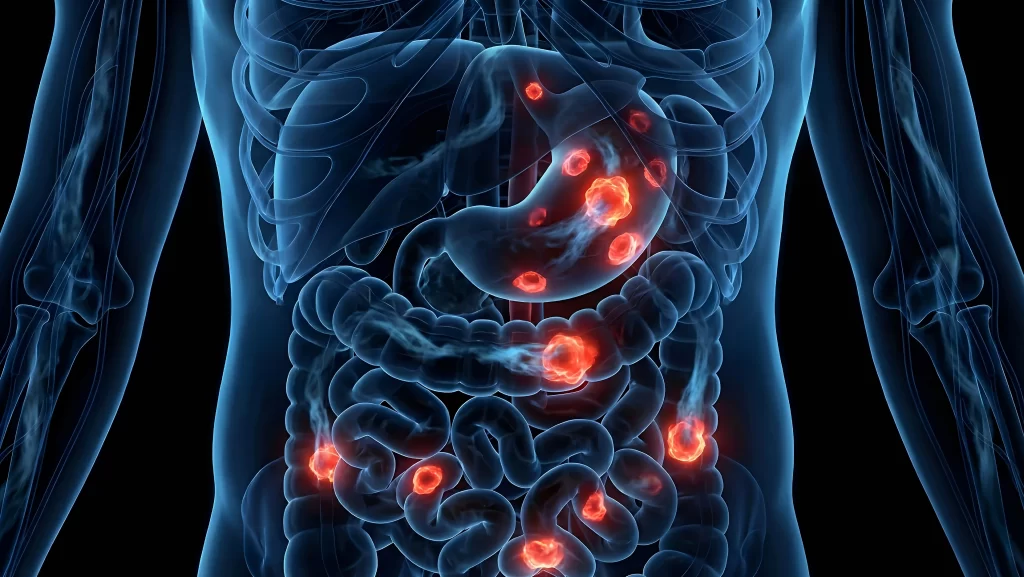
Neuroendocrine neoplasms (NENs), also known as neuroendocrine cancers, a broader medical classification used by specialists.
Neuroendocrine neoplasms (NENs) are broadly divided into two main categories:
Although they fall under the same umbrella, NETs and NECs behave quite differently and may require different treatment approaches. Knowing which type you have is important for planning the most appropriate care. If you are unsure about your diagnosis, speak with your oncologist for clarification.
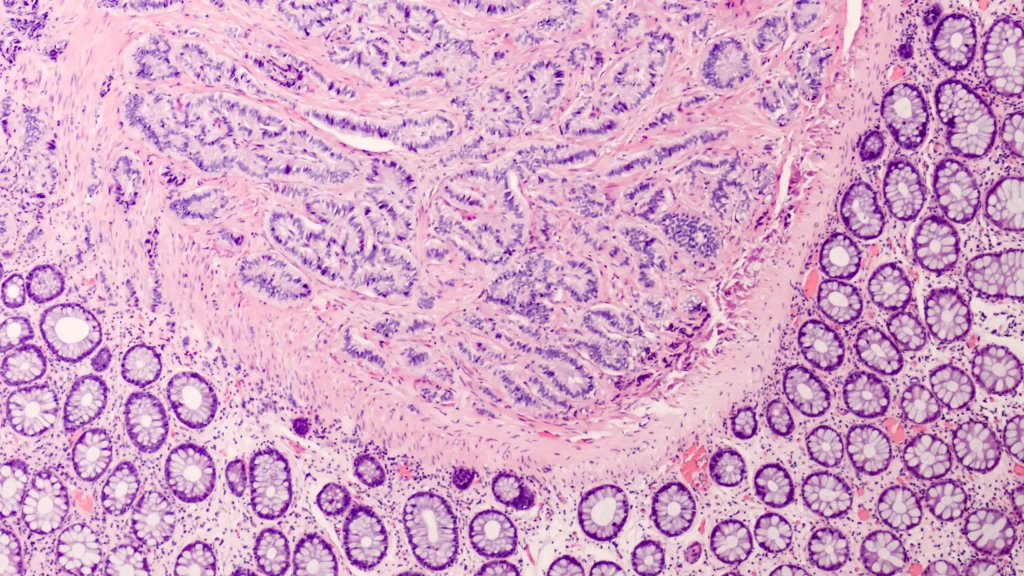
Pathologists evaluate tumour samples under a microscope to determine how similar the cells are to normal neuroendocrine cells and how quickly they are dividing. These features help classify the cancer and guide treatment decisions.
NETs are considered well-differentiated cancers. Although the cells are abnormal, they still retain some characteristics of normal neuroendocrine cells.
NETs are typically assigned a grade of 1, 2, or 3, which reflects how fast the tumour is growing, ranging from slower-growing to more rapidly growing forms. While lower-grade NETs often grow more slowly and may behave less aggressively, they are still considered cancers despite their slower growth and require appropriate evaluation and management.
NECs are poorly differentiated cancers, meaning the cells appear highly abnormal and no longer resemble normal neuroendocrine cells. They are generally classified by cell type, such as small-cell or large-cell variants. Unlike NETs, NECs are usually not given a formal grade because they tend to grow and spread quickly regardless of subtype.
Neuroendocrine neoplasms (NENs) are rare cancers in Singapore. However, their incidence has increased notably over the past two decades, with current estimates at approximately 2.4 to 2.5 cases per 100,000 people annually. These tumours most commonly arise in the gastrointestinal tract, particularly in the stomach, appendix, small intestine, and rectum.
Neuroendocrine neoplasms (NENs) may not cause noticeable symptoms in their early stages. Signs usually appear only when the tumour grows large enough to affect the normal function of an organ. As a result, symptoms can differ depending on the type of tumour, its grade, and where it is located in the body.
Possible symptoms may include:
These symptoms are common to many non-cancerous conditions, so their presence does not necessarily mean cancer. However, if symptoms are persistent, worsening, or unexplained, it is advisable to seek medical advice for proper evaluation.
Because the early symptoms of neuroendocrine neoplasms (NENs) can be vague and may overlap with many other medical conditions, reaching a diagnosis can take time. If a neuroendocrine neoplasm is suspected, your doctor may recommend specific tests based on the tumour’s possible location, type, and whether it is producing hormones.
Laboratory tests may be used to check for abnormal levels of certain hormones, enzymes, or proteins in the blood or urine. These tests can help detect neuroendocrine neoplasms (NENs), particularly those that produce excess hormones.
Imaging studies such as CT scans, MRI scans, or X-rays are commonly used to identify tumours within the body. PET scans may also be carried out to assess whether the cancer has spread to other areas.
Endoscopic procedures allow doctors to examine the inside of the body using a thin, flexible tube with a camera. Tissue samples can also be taken during the procedure. The type of endoscopy performed depends on where the tumour is suspected, such as an upper gastrointestinal endoscopy or colonoscopy.
In some cases, ultrasound imaging is combined with endoscopy to obtain clearer views of internal organs. This technique is often used to evaluate suspected neuroendocrine tumours in areas such as the pancreas.
A biopsy is performed to confirm the diagnosis. During this procedure, a small sample of tissue or fluid is collected and examined under a microscope. This analysis confirms the presence of cancer and provides information about the tumour subtype and how aggressive it may be.
In most people, the exact cause of neuroendocrine neoplasms (NENs) is not known. However, a small number are associated with inherited genetic conditions that can increase the risk of developing these tumours.
This group of conditions leads to the formation of tumours in various glands of the endocrine system. MEN type 1 (MEN1) is the condition most commonly associated with NETs, particularly pancreatic neuroendocrine tumours.
This inherited condition increases the risk of both benign and cancerous tumours in different parts of the body.
This disorder causes tumours to grow along nerves and on the skin, and may also affect the eyes and other organs.
A condition that can cause non-cancerous tumours to develop in multiple areas of the body, most often in the brain.
This syndrome is associated with benign growths and a higher risk of certain cancers.

Staging describes how far a tumour has spread in the body. For neuroendocrine neoplasms (NENs), staging may vary depending on the tumour’s location and subtype. In general, Stage 1 to Stage 4 are used, with higher stages indicating more advanced disease.
Grading refers to how the tumour cells look under a microscope and how quickly they are growing, which helps doctors assess how aggressive the tumour may be.
These tumours have cells that still resemble normal neuroendocrine cells and typically grow more slowly. Most Grade 1 and Grade 2 NETs fall into this category.
These cancers appear more abnormal and behave less like normal cells. They tend to grow and spread more rapidly and are often classified as higher-grade tumours, including many Grade 3 NETs.
Understanding both stage and grade helps guide treatment planning and provides information about prognosis.
Surgery is often the primary treatment for neuroendocrine neoplasms (NENs), particularly when the tumour is localised and can be safely removed. When tumours are larger, cannot be completely removed, or have spread to other parts of the body, additional treatments may be recommended.
在新加坡 OncoCare,我們的跨領域團隊成員包括專精於消化道及肝膽系統癌症的醫學腫瘤科醫師、擅長進行複雜及微創手術的肝臟外科醫師、放射腫瘤科醫師、放射科醫師、病理科醫師、腫瘤科護理師、營養師,以及腫瘤心理諮商師。他們齊心協力,為每位患者量身打造專屬的治療計畫。
如果您有風險因素或症狀顯示可能患有肝癌,請及早向我們的專家諮詢。及時診斷可提供有效治療和改善療效的最佳機會。